This Site Is A Participant In The Amazon Services LLC Associates Program. We may earn money or products from Amazon or the companies mentioned in this post.
There is no definitive answer to this question as there is no clear link between diabetes and acne. However, some studies have suggested that there may be a connection between the two conditions, though the exact nature of this connection is unclear. It is possible that high levels of blood sugar may contribute to the development of acne, or that certain medications used to treat diabetes can cause skin problems including acne.
If you are concerned about your risk for developing acne, speak with your doctor about your specific situation.
If you have diabetes, your body has trouble regulating blood sugar levels. This can cause a variety of skin problems, including acne.
Acne is a common skin condition that occurs when the hair follicles become plugged with oil and dead skin cells.
When these plugs form, bacteria can grow and cause inflammation.
Diabetes can make acne worse because high blood sugar levels can increase the amount of oil produced by the sebaceous glands. In addition, insulin resistance can lead to inflammation throughout the body, including the skin.
If you have diabetes and are struggling with acne, there are a few things you can do to manage your condition and help clear your skin:
-Keep your blood sugar under control: This will help reduce oil production and inflammation. -Use gentle cleansers: Harsh scrubs or soaps can irritate the skin and make acne worse.
-Choose non-comedogenic products: These products won’t clog pores or worsen acne.
What causes acne and how you can prevent it?
What Does Diabetes Acne Look Like?
If you have diabetes, you may experience certain skin problems—including acne. Here’s a closer look at what diabetes acne looks like and how it differs from regular acne.
Acne is a common skin condition that occurs when your hair follicles become plugged with oil and dead skin cells.
Acne most often appears on the face, neck, chest, and back. It can range from mild to severe.
While anyone can get acne, people with diabetes may be more prone to developing it.
That’s because high levels of blood sugar can trigger inflammation in the body, which can lead to skin problems like acne.
Diabetes acne may look different than regular acne. For starters, it tends to occur in adults rather than adolescents or teenagers.
And instead of being limited to the face, it can also appear on other areas of the body—like the neck, chest, and back.
What’s more, diabetes acne may be more likely to leave behind scars. That’s because inflammation associated with diabetes can damage skin tissue and make it harder for wounds to heal properly.
Can Blood Sugar Levels Cause Acne?
There is a lot of misinformation out there about the relationship between acne and blood sugar levels. So, let’s set the record straight: yes, blood sugar levels can cause acne.
When your blood sugar levels are high, it causes your body to produce more insulin.
Insulin is a hormone that helps regulate blood sugar levels. However, when too much insulin is produced, it can lead to a condition called hyperinsulinemia. Hyperinsulinemia has been linked to an increased risk for developing acne.
How does this work? Well, when insulin levels are high, it triggers your body to produce more testosterone. Testosterone is a hormone that plays a role in the development of acne.
So, when you have too much insulin in your body, it leads to an increase in testosterone production, which can then cause breakouts.
In addition to causing an increase in testosterone production, high insulin levels also promote inflammation throughout the body – including the skin. This inflammation can further contribute to the development of acne lesions and make existing breakouts worse.
So if you’re struggling with breakouts, it’s important to keep your blood sugar levels under control. Eating a healthy diet and maintaining a regular exercise routine can help stabilize blood sugar levels and reduce your risk for developing acne.
Can Diabetes Cause Skin Problems?
If you have diabetes, your body has trouble using the sugar in your blood. This can cause a host of problems, including skin problems. In fact, skin problems are one of the most common complications of diabetes.
There are several ways that diabetes can cause skin problems. High blood sugar levels can damage the tiny blood vessels in your body, including those in your skin. This damage can lead to dry, itchy skin and slow healing wounds.
Diabetic neuropathy (nerve damage) can also cause dry skin and make it harder for you to feel when you have an injury or wound. High blood sugar levels can also feed fungus and bacteria, leading to infection. Skin problems associated with diabetes include:
* Dry skin
* Itching
* Slow healing wounds
* Bacterial infections
* Fungal infections
What Do Diabetic Skin Problems Look Like?
There are a few different types of skin problems that can be associated with diabetes. One of the most common is called diabetic dermopathy, which appears as small, scaly patches on the skin. They are usually red or brown and most commonly appear on the legs.
Another common skin problem is called necrobiosis lipoidica diabeticorum (NLD), which appears as yellowish-brown plaques on the skin. NLD is most commonly found on the shins and ankles. Other less common skin problems associated with diabetes include eruptive xanthomatosis and digital sclerosis.
Eruptive xanthomatosis typically appears as raised, red bumps filled with pus that can occur anywhere on the body but are often seen on the back, buttocks, arms, and legs. The bumps eventually turn yellow or brown and harden. They may be itchy or painful.
Digital sclerosis refers to thickening and hardening of the skin on the fingers or toes, which can lead to joint deformities. The skin may also crack and bleed easily.
If you have diabetes, it’s important to watch for any changes in your skin and to see a dermatologist if you develop any new bumps or growths.
Credit: www.aad.org
Can Type 2 Diabetes Cause Acne?
There is no definitive answer to whether or not type 2 diabetes can cause acne. However, there are some potential mechanisms by which diabetes could theoretically worsen acne. For example, high blood sugar levels can lead to inflammation throughout the body, and this inflammation can in turn worsen acne.
Additionally, certain medications used to treat diabetes (such as corticosteroids) can sometimes cause side effects that include acne breakouts.
Of course, it’s also possible that type 2 diabetes and acne are simply unrelated conditions. Some people with type 2 diabetes may experience worsened acne while others do not; it really depends on the individual.
If you’re concerned about your acne worsening after being diagnosed with type 2 diabetes, be sure to discuss your concerns with your doctor so they can help you determine if there’s anything you can do to manage both conditions effectively.
Cure of Diabetes Acne
There are many different treatments for acne, but there is not necessarily a cure. However, some treatments may be more effective than others in certain cases. For example, isotretinoin (commonly known as Accutane) is often prescribed for severe acne that does not respond to other treatments.
This medication can help to prevent further breakouts and can also reduce the size and severity of existing pimples. In some cases, it may even be possible to completely clear the skin using this medication. However, it is important to note that isotretinoin can have serious side effects, so it should only be used under the supervision of a qualified healthcare provider.
Diabetes Rash on Legs
If you have diabetes, you may experience a range of skin problems. One common issue is a rash on your legs. This can be a frustrating and embarrassing problem, but it’s important to know that there are treatments available.
There are several different types of rashes that can affect people with diabetes. The most common is diabetic dermopathy, also known as shin spots or pigmented purpuric dermatosis. This rash appears as small, dark spots on the shins or lower legs.
It’s usually painless and doesn’t itch.
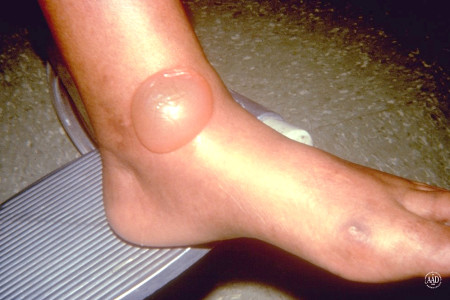
Another type of rash is called diabetic blisters (bullous diabetique). These blisters can occur on the feet and toes, hands and fingers, or any other area of the body where there’s friction or rubbing.
They’re filled with clear fluid and usually don’t cause any pain unless they break open.
If you have either of these types of rashes, it’s important to see your doctor so they can rule out other possible causes and determine the best course of treatment. In most cases, these rashes can be managed with topical creams or ointments and by keeping your skin clean and well-moisturized.
More severe cases may require oral medications or light therapy.
No matter what type of diabetes rash you have, it’s important to take good care of your skin overall.
Conclusion
There are many potential causes of acne, and diabetes may be one of them. High levels of blood sugar can lead to inflammation and changes in hormone levels, both of which can trigger acne breakouts. If you have diabetes and are struggling with acne, talk to your doctor about possible treatments.